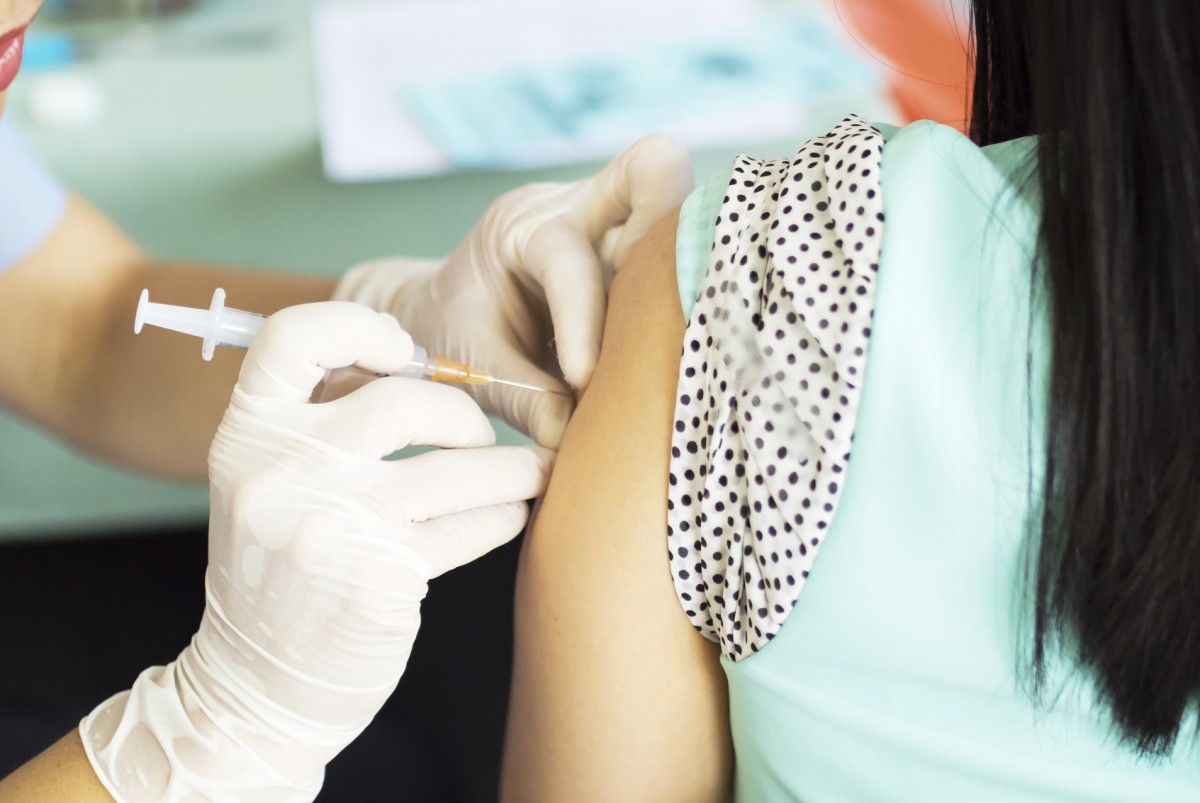
I was first offered the HPV vaccine during my college years. Although I had been counseled about the importance of the vaccine at that time, the steep price for the three-vaccine series kept me from getting it. With each injection costing $190, it was simply something I could not afford. By the time I started medical school in 2009, my insurance started covering the vaccine for women my age, so I elected to get it. My new classes had just started, and I was learning more about cervical cancer and its association with HPV.
Recently, almost seven years after my last shot of the series, I started to wonder how many teenagers are getting these shots. Surely the increase in insurance coverage of the HPV vaccine would increase the vaccination rate, helping more young individuals become vaccinated, as it had with me.
After taking care of my first patient with cervical cancer during my fourth year of medical school, I realized that although we have made leaps and bounds in cervical cancer screening, we have so much left to do in terms of preventing this disease. My patient was only a few years older than me. For her, one abnormal Pap smear a few years before was all she needed to develop cervical cancer. By then, it was too late. She had a tumor encompassing the entirety of her cervix that kept her from urinating as much as she should. The mass was already compressing her other organs, and her kidneys were starting to fail.
Currently in the U.S., only about 63 percent of girls and 50 percent of boys nationwide have been vaccinated. Even so, it has been harder for me to convincingly explain the importance of the HPV vaccine to some of my younger patients than it is for other standard vaccinations. It takes relatively little effort to convince a patient why a flu shot or a chicken pox vaccine is important. Most people can see the effects of these illnesses on people around them and want to prevent them. Comparatively, cervical cancer is a silent disease; it’s nowhere near as common as diseases like the flu, and even those who do develop the disease rarely display symptoms.
While most people generally do not like their health controlled by lawmakers, some states and health departments have tried to set mandates for middle school-aged children to get vaccinated before they start seventh grade. The first state to do this in 2007 was our neighboring Virginia. Unfortunately, even mandatory vaccination did not lead to increased uptake of the vaccine among school-aged girls. This same trend has been seen in many states that have tried to introduce bills for mandatory vaccination. However, provider counseling of parents and their children about the HPV vaccine has been shown to increase vaccination rates. In light of such findings, it’s up to us as providers to do better.
Related Content
- Creating Vaccines to Kick Cancer’s Butt. Watch now.
- Cervical Cancer Research Lab
- If You Feel Something, Say Something: Preventing and Detecting Gynecologic Cancers
- Vaccine Clears Some Precancerous Cervical Lesions in Clinical Trial