For many obese people, losing and maintaining weight is a constant struggle. It often takes several months of careful dieting and exercise to see results, but those stubborn pounds frequently come back within weeks. One of the common causes of this cyclical pattern of weight gain is that the body can respond to calorie restriction by drastically reducing its metabolic rate. Bariatric surgery is often promoted as an option for such people.
What is Bariatric Surgery?
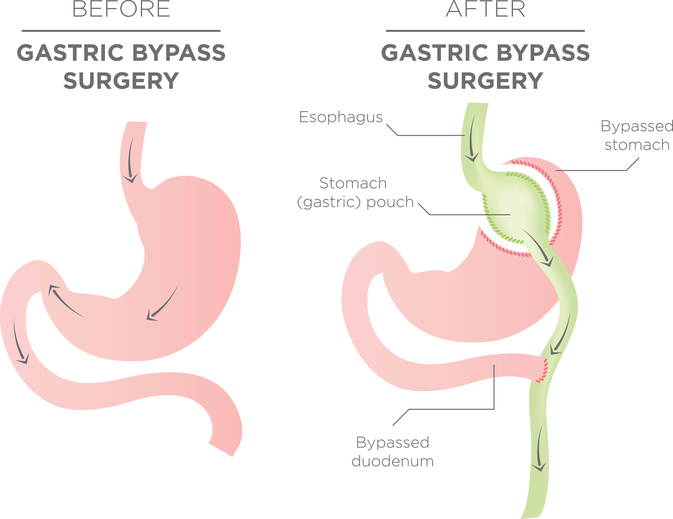
Bariatric surgery includes reducing the size of the stomach, either with a gastric band, which reshapes the stomach to create a small pouch and bypassing a portion of the stomach (gastric bypass), or by removing a small portion of the stomach altogether (sleeve gastrectomy). Both procedures can cause corresponding changes in the small intestine as well. These procedures spur weight loss by restricting the amount of food the stomach can hold, increasing feelings of fullness and reducing the absorption of nutrients. It has been observed that bariatric surgery has beneficial effects not only for treating obesity, but for type 2 diabetes as well.
Can Bariatric Surgery Benefit Patients with Diabetes?
A recent study lead by Philip Scheuer of Cleveland Clinic looked at long-term (five-year) outcomes of a clinical trial that compared bariatric surgery versus medical therapy. The patients were randomly divided into three groups — a bariatric surgery group treated with gastric bypass and provided with diet support, a bariatric surgery group treated with sleeve gastrectomy and provided with diet support, and a medical therapy group that involved keeping track of medication and education about diet and exercise related to diabetes. The study, named STAMPEDE (Surgical Treatment and Medications Potentially Eradicate Diabetes Efficiently), was published in the Feb. 16 issue of The New England Journal of Medicine and indicated that compared to those with diabetes who followed medical therapy, patients who underwent gastric bypass showed more significant improvements in glycemic control.
The study included 150 patients with an average age of 49 years, average body mass index of 37 and an average glycated hemoglobin level (HbA1c) of 9.2 percent. HbA1c is a clinical measurement used to assess blood sugar levels and is considered the gold standard for monitoring glycemic control in patients with diabetes. Patients with an HbA1c below 6 percent are considered healthy, whereas a result between 6 and 6.4 percent is an indicator of prediabetes, and anything above 6.5 percent is diabetes. The patients were randomly assigned into two groups — one underwent either gastric bypass or sleeve gastrectomy, and the other received medical therapy alone. The goals were to monitor their HbA1c levels and to lower HbA1c levels to 6 percent or below, which is indicative of well-controlled diabetes.
Study Findings
After five years of follow-up, 5 percent of the medical therapy-only group had achieved an HbA1c level of 6 percent or less, whereas 29 percent of the surgical intervention group had reached this goal. Patients who underwent surgery also showed other improvements, such as losing significantly more weight, more significant reductions in waist circumference, dramatically lower triglycerides and cholesterol levels, and better quality of life than those who were treated with medication alone.
Although the observation that patients with type 2 diabetes have better glycemic control after bariatric surgery is not new, most studies until now were observational and included only severely obese patients. The current study is the first randomized controlled study of this scale. Another important conclusion from this study involved patients with body mass index between 27 and 34. Most insurance companies will cover bariatric surgery for people with a body mass index of 40 or higher, or alternatively, 35 or higher (in the presence of other comorbidities). However, this study shows that even patients with a body mass index of 27 to 34, significantly below these cutoffs, benefited from the procedure as compared to those with medical intervention alone.
Lastly, the study found that gastric bypass led to greater weight loss with fewer diabetic medications and thus appears to have an advantage over sleeve gastrectomy. However, the authors caution that their trial was not designed to detect other small but clinically significant differences between the two procedures. There might be additional advantages of gastric bypass over sleeve gastrectomy that might be uncovered by trials designed to address those questions specifically.
References
Bariatric Surgery versus Intensive Medical Therapy for Diabetes — 5-Year Outcomes
Bariatric surgery procedures
A Guide to HbA1c
Related Content
- Body Contouring After Weight Loss: What You Need to Know
- Learn more about weight loss services available through the Johns Hopkins Digestive Weight Loss Center