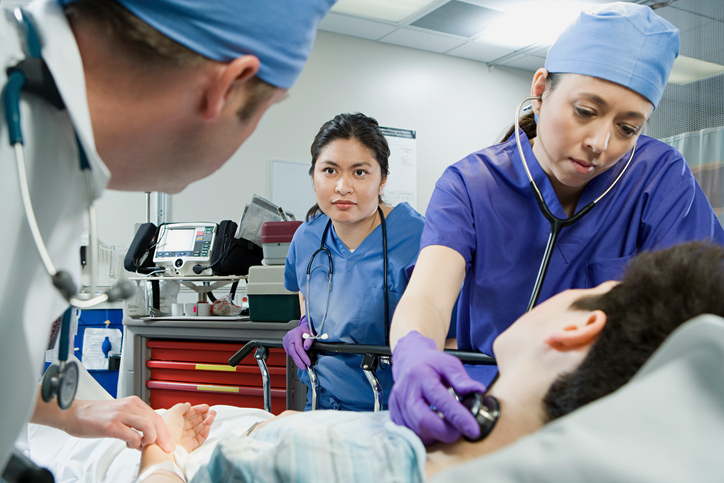
Seven medical students shuffle through the narrow doorway. One of my classmates steps forward and addresses the patient. “Hello, Mr. M. How are you doing this morning?”
Mr. M. does not respond.
“Mr. M.? Mr. M.?” The student shakes the patient’s shoulder vigorously. The student feels for a pulse. “I have a pulse, and I see chest rise.” We all release half a breath: The patient is not in cardiac arrest. But why can’t Mr. M. respond?
Fortunately, Mr. M. is not in any danger because Mr. M. is a mannequin. But this is no mere plastic simulacrum. Mr. M. really does have a pulse. He has lungs that inflate to lift his chest. He can be shocked, intubated and examined for neurological deficits. Mr. M. is a $100,000 machine built for simulating emergency medicine. And he is also a forgiving instructor to green second-year medical students just learning to translate textbook medicine to the hospital bedside.
Medical school is traditionally divided between two years of classroom-based instruction in physiology and the mechanism of disease, and two years of hospital-based training. On the wards, medical students rotate through each of the core specialties for several weeks at a time: internal medicine, surgery, pediatrics, obstetrics/gynecology, neurology and psychiatry. The transition between these two phases of medical education is, unsurprisingly, associated with significant intellectual and emotional shock. Students are no longer full-time learners solely responsible for expanding their own knowledge. In the hospital, they become active participants on the medical care team, accountable to patients and professional colleagues as well as to their own learning.
 To better prepare soon-to-be third-year students for the rigors of hospital medicine, the Johns Hopkins faculty developed the Transition to Wards course. The three-week class concentrates its efforts on common early stumbling blocks faced by medical students. Students review the interpretation of frequently used diagnostic tests, revisit the principles of biomedical ethics, train in basic procedural skills and learn the steps for initial management of an acutely ill patient.
To better prepare soon-to-be third-year students for the rigors of hospital medicine, the Johns Hopkins faculty developed the Transition to Wards course. The three-week class concentrates its efforts on common early stumbling blocks faced by medical students. Students review the interpretation of frequently used diagnostic tests, revisit the principles of biomedical ethics, train in basic procedural skills and learn the steps for initial management of an acutely ill patient.
At this stage of education, it’s all about introducing and drilling in the basics. Mnemonics are (literally) lifesaving tools used to bridge the gap between learning a medical principle and internalizing it. One classic for acute care: “When a patient is sick, say ‘OMI!’—oxygen, monitoring and IV access.” The transition course provides room for mistakes without human consequence during the steepest part of the learning curve.
Why can’t Mr. M. respond? Oxygen and monitors are hooked up, and the IV is open. He is not in cardiac arrest. Heart rate, respiratory rate and blood oxygenation look good, but his blood pressure is concerning at 144/80. Two years of pathophysiology kicks in. My teammates call out potential causes for unconsciousness, and side conversations instantly spring up, each pair or trio debating a different diagnosis. Another classmate, silent until now, suggests in a clear, crisp voice that we check a finger stick blood glucose.
I want to high-five her for her insight: Low blood sugar is one of the most common causes of nonresponsiveness — obvious in retrospect, but it’s astonishing how few concepts are obvious to a medical student struggling to diagnose an active problem. We check the blood sugar; it’s a third of what it should be. We give glucose, and slowly, Mr. M. comes to.
A small victory, perhaps. Hypoglycemia is not a difficult or complex diagnosis. But a team of my classmates examined, diagnosed and treated a simulated patient for a potentially lethal condition. My classmates saved a life. That’s enough to put a spring in my step.
Related Content
- Find out more about the Transition to Wards course program.
- Learn more about medical student programs in emergency medicine.