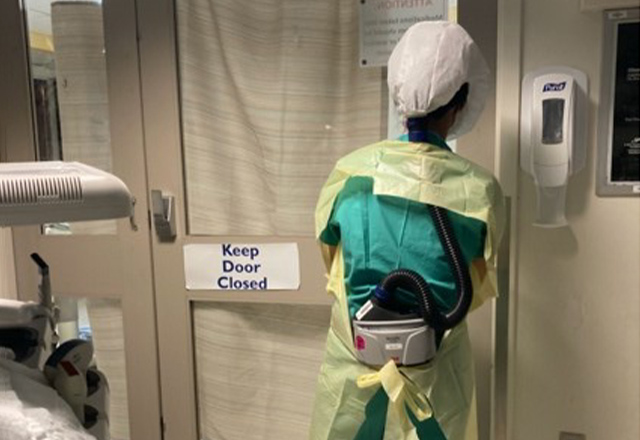
(Photo caption: A hospital employee stands outside one of the COVID-19 rooms at Johns Hopkins Bayview Medical Center. Photo courtesy of the author.)
Every year, a new crop of internal medicine, psychiatry and neurology interns at Johns Hopkins Bayview Medical Center are tasked with creating an oath — a “North Star” to help guide us through three (or more) years of residency. Most years, the oath serves to reaffirm the incoming interns’ collective commitment to humanism and professionalism. But this year, there is a new underlying force that will shape most, if not all, of our residency experience: COVID-19.
Here is just a small piece of this year’s oath, as it relates to the current pandemic:
“During this challenging time of the COVID-19 pandemic, we vow to keep you (our patients) safe and strive to transcend both physical and emotional barriers that exist between you, your health care providers, and your loved ones.”
This promise to our patients may seem straightforward. Of course, as doctors, we strive to ensure patient safety. During the pandemic, however, we have to be especially cautious to practice medicine without losing the human connection.
One of the hardest parts of working in medicine during COVID-19 is building a rapport with patients while wearing masks, gowns and face shields. These physical barriers, while no doubt necessary, also prevent patients from seeing and feeling our nonverbal signs of empathy and mutual respect. One way I have found to overcome this limitation is to show all of my patients my ID badge as soon as I meet them so they can see that I do, in fact, have a face. I also have a low threshold for sharing personal photos from my phone to give them a better sense of my life outside of the hospital as well as my interests and hobbies beyond medicine.
Another way to transcend these physical barriers is to encourage and facilitate face-to-face communication between patients and their loved ones using FaceTime, Zoom and other technological aids. When we are able to arrange a virtual visit with a patient’s family, they usually immediately perk up and smile at the sight of their loved ones.
Connecting patients with dementia to their family members has enormous therapeutic value. In 2017, a special issue of Aging & Mental Health encouraged the use of social health as a tool for managing dementia and emphasized the need for more interventions that help people with cognitive disabilities maintain their social networks and relationships.
But our efforts to transcend physical and social barriers during COVID-19 should not stop with personal photos and video visits. While working in the medical ICU, one of the most meaningful things I have done has been to keep family members updated on the status of their loved ones and, together with the nursing staff, obtain visitation privileges for family members in the hours immediately preceding a patient’s death. Nobody should have to die alone, and we owe it to our patients to let them be with their loved ones before they pass.
But where do we draw the line? As employees of a hospital, it is our duty to protect our patients from acquiring communicable diseases from others around them. This is a difficult question that hospital administrators and infection control experts must be grappling with every day. But even during “lockdown” periods when physical barriers are necessary, it is important to remember that there are still things we can do — like sharing personal photographs or arranging virtual family visits — to help build more human connections for and with our patients.
Related content
- Fifteen Minutes of Companionship
- Learning to Grapple with Difficult ‘Firsts’ in Medical Training
- Resuming Medical Training in the Era of COVID-19: A Medical Student’s Thoughts
Want to read more from the Johns Hopkins School of Medicine? Subscribe to the Biomedical Odyssey blog and receive new posts directly in your inbox.