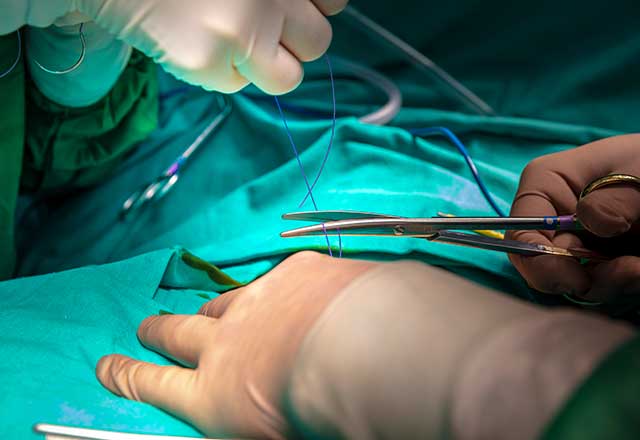
For me, one stitch down, many to go. Start the new stitch at the same level you just came out of. Load the needle driver again before you pull the needle out all the way. It’ll save time. Use the Adsons to pull the tissue up, not over. UP, not over. Go as deep as you did for the stitch before. Keep it consistent. That’s right. Pull it tight, the epidermis should meet when you do. Wow, it’s actually looking good. Don’t mess up. Don’t get scared. Just keep going. They’ll fix it if it’s messed up. Just keep going.
A Reminder
My mask caught the tear that lightly rolled down my cheek as I sutured a woman’s chest after her mastectomy. One stitch at a time, I helped minimize the scar that would make where her breast used to be — a scar that she will always remember. A scar that will serve as a reminder of the battle she fought against breast cancer. A scar that will be discernable, present and immediately in view every time she undresses. A scar that my mother bears as well. That scar is the reason I am here, suturing carefully and calmly.
When I began my surgery rotation as a third-year medical student, I was placed into the service that treats breast disease. While I looked forward to it greatly, a part of me was nervous, frightened and worried about how I would feel seeing my mother in every patient. Medical training prepares you to diagnose, to treat and to follow-up, but nothing prepares you for being in the moments you don’t want to relive.
An Ongoing Battle
I was 10 years old when my mother was diagnosed with stage 2 breast cancer. Her aggressive histology was responsible for her aggressive treatment plan. Her spontaneous lymph node involvement was responsible for the years during which we felt fear. But her relationships with her physicians is the reason I am here in medical school today. While that may help me understand patients with cancer earlier in my career than most, it brings back memories that make me hesitate before I can walk into the room. I know that when these women leave the hospital, they go home to watch their hair shed — slowly, but in chunks. I know they’ll have nights of vomiting, days of fatigue, painful mouth sores, and the ever-present frustration with not being able to recognize themselves when they look in the mirror. Everything changes: appetite, weight, mood and — I remember as I help finish up the surgery — the body itself. One of the worst parts about fighting cancer is that patients are fighting it in a body they don’t recognize, a body that has become generally weak and physically scarred. They’re enduring excruciating treatments that make them question whether it’s worth it to continue the course or just give up and let the cancer triumph. And the cruelest part of that, is even if they do wake up and choose to battle every day, there’s always the gamble the cancer will succeed anyway.
As I crack open the Dermabond like a glowstick, I remember to never judge my future patients for the choices they make at a time when they are fighting physically and emotionally. I remember the families supporting each cancer patient and praying for their recovery, just as I did for my mother. I remember how lucky I am to be a part of one of the most formative experiences of their lives. I pull off my gown and gloves and stand in silence as the patient is rolled out of the OR. For her, one treatment down, many to go.
Related Content
- Foghorn Therapeutics Breaks New Ground in Cancer Epigenetics
- Next Generation Cancer Diagnostics Revolutionize Patient Care
- Oncology: Offering Hope to Patients in Need
- Everyday Antibiotics May Reveal New Therapies to Treat Your Breast Cancer
Want to read more from the Johns Hopkins School of Medicine? Subscribe to the Biomedical Odyssey blog and receive new posts directly in your inbox.