In cardiac surgery, most patients come out of the operating room still heavily sedated and intubated — a tube down their windpipe helps them breathe, one is in their bladder so they don’t need to urinate and multiple others protrude from their chest, draining blood-tinged fluid. Some patients exit surgery actively “paced,” with several wires on the surface of their heart urging it forward at a steady rhythm somewhere between 90 and 100 beats per minute. The first six hours after open-heart surgery are crucial, so patients are quickly wheeled from the operating room to the cardiovascular surgical ICU — also known as the CVSICU — where they are closely monitored during this critical recovery period.
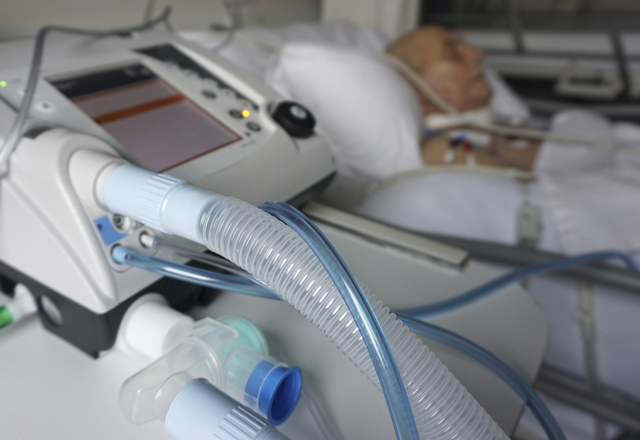
As you might imagine, the CVSICU can be overwhelming for patients’ loved ones and the patients themselves. As they are gradually weaned off sedating medications, patients often awake to a choking sensation from the breathing tube forcefully blowing oxygenated air into their lungs. One family member once mentioned that the scariest part for their loved one wasn’t the thought of having his sternum split open by a bone saw to expose his heart for surgery; he was most afraid of waking up on a ventilator. Thankfully, for most patients, “wake, wean and extubate” is the typical plan for post-surgical recovery. As their sedatives are reduced, most patients can understand and follow commands, and are able to easily have the tube removed and breathe on their own.
All fourth-year medical students at Johns Hopkins undergo a one-month rotation in critical care to better understand and learn how to care for complex patients. Over the last month, I was intimately involved in the care of several patients whose post-recovery plans required extra time on the ventilator during my rotation in the CVSICU. A few of these patients experienced a phenomenon called ICU delirium. Delirium refers to a state of altered thinking and consciousness that can occur in the critically ill patient. Patients often become confused, disoriented and agitated following a major surgery or while recovering from trauma. In such cases, delirium can induce an altered state of reality, as the sounds and sights of the ICU interact with the patient’s own thoughts to create terrifying and bizarre illusions. Because of the instability and agitation that often coincide with ICU delirium, these patients are kept on the ventilator for longer to protect their airways and support breathing.
“She wasn’t herself,” said one family member as she reflected on her mother’s ICU stay. “At first, it looked like she was getting worse instead of better.”
Delirium is associated with psychological distress, such as PTSD, and poor health outcomes, including longer ICU stays and higher rates of mortality. Therefore, it is critical that CVSICU staff members be especially vigilant in monitoring and treating delirium. Indeed, one study from 2010 found that over 80 percent of patients on ventilators at a particular institution experienced ICU delirium. Johns Hopkins is taking steps to find better ways to treat and support patients who go through delirium in the ICU, including orienting patients to a day-night cycle with natural light, using sedating medicines sparingly and monitoring patients’ mental states post-surgery using delirium screening tools. By combining psychological and physical rehabilitation and supporting patients throughout the recovery process, it is the hope of researchers that the incidences of ICU delirium can be reduced to improve patient outcomes.
Read More »The Problem of Delirium in the Intensive Care Unit